Gas and bloating can be horribly uncomfortable and embarrassing. I recently suffered from a horrific bout on a trip to Korea. In trying to get my 6–8 vegetable servings a day, I ate whatever Korean vegetables were available — the vast majority of which were fermented.
I love kimchi and pickled onions, but I do not eat gobs of them regularly, and boy, that set off my system!
Talk about a superpower — who else can clear a room in 2 seconds flat?
There are many causes of gas and bloating.
The most obvious one is eating WAY too much gas-producing food — cabbage and onions (go figure), but beans and lentils are also huge culprits.
Gas and bloating can also be from:
– Swallowing too much air when you eat. This can occur if you are rushing to eat or drink, talking with your mouth full, using straws, or drinking carbonated beverages.
– Eating lots of high-fiber foods. This is especially true if you suddenly ramp up your dietary fiber and your system and microbiome don’t have a chance to adjust. This is not to say that you shouldn’t be eating your fiber, but rather, I encourage you to increase your servings gradually.
– Eating foods you can’t digest well. These include lactose (Asians are very familiar with this!), fructose, and artificial sweeteners. These sugars are generally not well absorbed and lead to gas and often diarrhea.
– Digestive disorders, such as irritable bowel syndrome or inflammatory bowel disease.
– Inadequate digestion — not chewing your food well or having insufficient digestive enzymes to break down food. You may have these issues due to rushed eating or stress, but underlying medical conditions, such as poor dentition, pancreatic problems, or liver and gallbladder issues, may also cause them.
– Constipation — big one (pun intended)! Not having at least one bowel movement daily can lead to backup and bloat.
– Infections — parasites or other microorganisms can be culprits.
– Medications — some medications may be contributing to your symptoms.
Examples include:
o Antibiotics, which alter your gut microbiome
o Iron can cause constipation
o Some antidepressants may alter your gut motility
o Opioids slow down your digestive tract
o Antacids or proton pump inhibitors reduce stomach acid, which can affect digestion.
o Cardiac and diabetic medications can also sometimes cause gut side effects.
– And finally, another culprit of gas and bloating is SIBO — small intestinal bacterial (or fungal) overgrowth. This is the one I am going to highlight today.
What exactly is SIBO, and do I have it?
First, let’s start with a little bit of background.
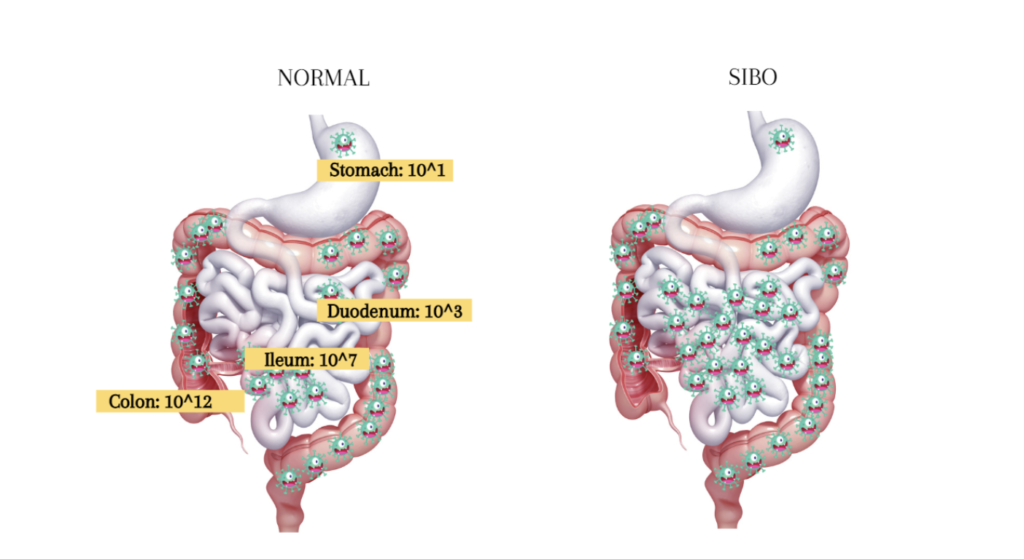
In our gut, we have trillions of microorganisms. Most of these microorganisms live in our large intestine or colon (the pink part in the diagram above). But we also have microorganisms throughout our intestinal tract, starting in the stomach. The stomach is an acidic, hostile environment; therefore, usually, we only have a small number of microorganisms that can survive there.
After the stomach, we have the small intestine, starting with the duodenum. The environment here is not as acidic, although pancreatic digestive enzymes, bile, and the migrating motor complex keep the population of microorganisms down.
The migrating motor complex is a coordinated series of contractions that involve the stomach and the small intestines. These contractions typically occur between meals and during fasting and sweep out the contents in the small intestine, pushing them into the large intestine.Effectively, this clears out food as well as microorganisms.
Now, we get to the large intestine. Here, things move much more slowly, and the contents sit in the colon anywhere from 12–48 hours. This is lots of time for microorganisms to throw a party and replicate without abandon!
What happens when things go awry?
If the above processes do not work normally, things can go wrong, and you can develop SIBO. SIBO occurs when you get an overgrowth of microorganisms in the small intestine.
Alterations in any of these areas can promote SIBO:
1. Inadequate stomach acid, pancreatic digestive enzymes, or bile secretion
2. Impaired motility or impaired migrating motor complex
3. Anatomical problems include post-surgical changes, scar tissue, or tissue laxity.
What symptoms are associated with SIBO?
SIBO can cause uncomfortable symptoms such as bloating, abdominal pain or discomfort, and gas. These symptoms are not specific to SIBO; many other conditions produce the same symptoms. A more serious concern with SIBO is that it can cause problems with malnutrition, either from a loss of appetite or malabsorption of nutrients.
How do you diagnose SIBO?
As I have noted, many other conditions also cause the common symptoms that occur with SIBO. A clinical and medical assessment will look for these different conditions, as well as SIBO.
– Blood or stool testing: to evaluate for inflammation or malabsorption. Depending on your medical history, to also rule out Celiac disease.
– Imaging: to evaluate other gastrointestinal conditions and the small intestine.
Specific testing for SIBO:
– Breath testing: this is the most common method used to diagnose SIBO, as it is non-invasive.
This test involves drinking a sugary substrate (either lactulose or glucose) and checking the production of hydrogen, methane, or hydrogen sulfide gas by the bacteria in the small intestine, which is measured through your breath. Elevated levels may indicate SIBO.
– Endoscopy. An endoscopy evaluating the upper small intestine may be performed in some cases. A sample can be obtained during this procedure to check the microorganism load in the small intestine.
So, it’s SIBO — how do you treat it?
SIBO can be treated with antibiotics or natural plant compounds and a low FODMAP (fermentable oligosaccharides, disaccharides, monosaccharides, and polyols) diet.
However, the key to long-term treatment of this condition is addressing the underlying cause — motility, digestion, and anatomy. Addressing these underlying causes will help prevent recurrences in the future.
If you suffer from gas and bloating, I encourage you to have a medical evaluation with your healthcare provider.
Things you can do in the meantime to help improve your digestive health:
1. Mindful eating. Enjoy your meals in a low-stress state and chew your food well.
2. Give your guts a chance to rest. The migrating motor complex is most active when we are not eating.
a. Aim for at least a 12-hour window of not eating (i.e., 7 pm to 7 am).
b. Minimize snacking between meals.
3. Consider a trial of limiting your intake of lactose and artificial sweeteners.
4. Consider temporarily cutting back on your fiber and then reintroducing fiber gradually. Cooked vegetables tend to be easier to digest than raw.
5. Get moving! The movement will also stimulate the activity of your guts!
Wishing you all a new year with no gas!
- Dr. Eri Shimizu
For more useful information on functional holistic health, you can visit our FREE video library here.
About the Author:
Dr. Eri Shimizu is a board certified in Internal Medicine Doctor and certified through the Institutes of Functional Medicine. She earned a Bachelor of Science in Environmental Bioengineering from the University of Hawaii at Manoa and graduated summa cum laude from Creighton University Medical School. She completed her Internal Medicine residency at UCLA and worked at a Los Angeles county hospital. In 2012, she returned to Hawaii and served as a Hospitalist at Maui Memorial Medical Center. Maui is now home with her husband, two children, and a fighting fish named Rainbow.
Schedule a FREE Functional Medicine Health Consult with Dr. Eri.









